Hepatic steatosis, also known as fatty liver disease, is becoming increasingly common in the United States, as well as on a global scale. To effectively prevent and reverse fatty liver disease, it’s important to understand the causal factors fueling its development. Is hepatic steatosis influenced primarily by genetic or environmental factors? It turns out that hepatic steatosis is influenced by a mixture of both.
What Happens When You Have Nonalcoholic Hepatic Steatosis
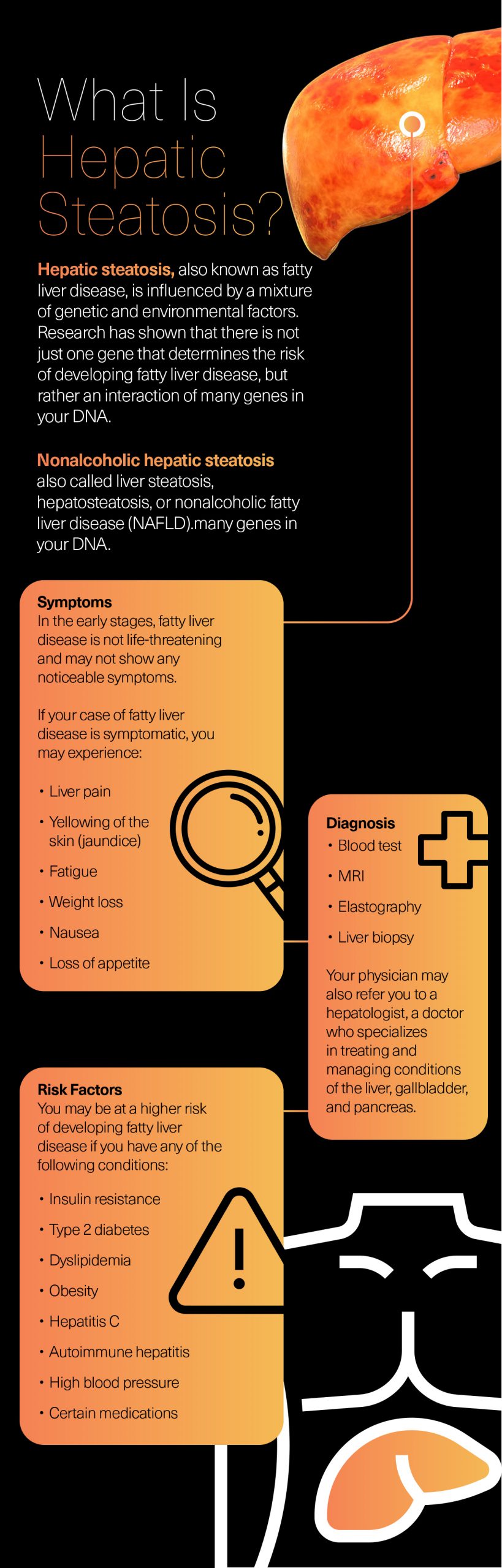
Nonalcoholic hepatic steatosis – also called liver steatosis, hepatosteatosis, or nonalcoholic fatty liver disease (NAFLD) – and describes the accumulation of fat in the liver that is not related to alcohol consumption. The terms “hepatic steatosis” and “fatty liver disease” can be used interchangeably.
Symptoms
In the early stages, fatty liver disease is not life-threatening and may not show any noticeable symptoms. If your case of fatty liver disease is symptomatic, you may experience:
- Liver pain
- Yellowing of the skin (jaundice)
- Fatigue
- Weight loss
- Nausea
- Loss of appetite
Diagnosis
Even if you have no symptoms, a physician can diagnose fatty liver disease based on clinical features. A diagnosis of fatty liver disease requires that 5% of hepatocytes – or liver cells – are carrying excess fat. Your physician will likely make your diagnosis based on a blood test that reveals elevated liver enzymes, including high levels of aspartate transaminase (AST), alanine transaminase (ALT), alkaline phosphatase (ALP), and gamma-glutamyl transpeptidase (GGT).
A diagnostic imaging test can confirm swelling and enlargement of the liver, as well as the presence of excess fat in the liver. A magnetic resonance imaging (MRI) test uses radio waves to reveal detailed information about hepatic fat levels. Elastography is a particular form of ultrasound imaging that yields diagnostic information about the liver. As the name suggests, elastography can assess the texture of liver tissue. Harder tissue suggests the presence of fat or inflammatory damage in the liver.
A liver biopsy may also help assess the level of inflammation present in hepatocytes. Your physician may also refer you to a specialist in the field of hepatology, also called a hepatologist. A hepatologist is a doctor who specializes in treating and managing conditions of the liver, gallbladder, and pancreas.
Risk Factors
Fatty liver disease usually does not occur in isolation. Many other health conditions related to metabolic functioning may occur simultaneously. Viral infections or genetic liver diseases may also increase the risk of developing hepatic steatosis. You may be at a higher risk of developing fatty liver disease if you have any of the following conditions:
- Insulin resistance: Insulin resistance occurs when your insulin stops responding normally to the presence of sugar in the blood.
- Type 2 diabetes: Over time, insulin resistance leads to type 2 diabetes, which leads to skyrocketing blood sugar levels and resulting tissue damage.
- Dyslipidemia: This condition means the lipid levels in the blood are abnormal. Abnormal serum lipid levels may encompass low levels of high-density lipoprotein (HDL) cholesterol, high levels of LDL (low-density lipoprotein), high levels of VLDL (very low-density lipoprotein) cholesterol, and high triglycerides.
- Obesity: Obesity is characterized by a body mass index (BMI) that is far above the normal range. Fat accumulation throughout the body increases the risk of fat accumulation in the liver.
- Hepatitis C: Inflammation related to the hepatitis C viral infection can increase the risk of fat buildup in the liver.
- Autoimmune hepatitis: Liver inflammation related to an abnormal immune response increases the risk of fat accumulation in the liver.
- High blood pressure: High blood pressure, or hypertension, is a vascular manifestation of metabolic syndrome and is correlated with heart disease.
- Certain medications: Certain chemotherapy drugs, like methotrexate, can alter hepatic processes and increase the likelihood of developing fatty liver disease.
Complications
If taken care of during these early stages, hepatic steatosis can be easily reversed. Issues arise if curative measures are not taken and fatty liver disease progresses to more life-threatening forms of liver disease. Progressed forms of fatty liver disease include:
- Nonalcoholic steatohepatitis (NASH): The presence of NASH indicates chronic inflammation in the liver that injures liver cells.
- Liver fibrosis: NASH, if left untreated, can lead to liver fibrosis, which describes the development of tough fibrotic tissue in the liver as a result of chronic inflammation-induced liver injury.
- Cirrhosis: When liver fibrosis continues for a long period of time, it can lead to liver cirrhosis, which describes the presence of hard scar tissue that reduces liver function.
- Hepatocellular carcinoma: Chronic damage to liver cells markedly increases the risk of developing hepatocellular carcinoma, also known as liver cancer.
- Liver failure: Years of liver damage can lead to liver failure, which describes the complete loss of liver function. At this stage, liver transplantation is the only viable form of treatment.
Causes of Nonalcoholic Hepatic Steatosis
Determining the causes of hepatic steatosis is crucial to successfully treating and reversing the condition, in order to prevent progression to more serious stages.
Fatty Liver Disease Has a Genetic Component
The likelihood of developing fatty liver disease is influenced in part by genetics. But the heritability of fatty liver is not so simple to determine. Research has shown that there is not just one gene that determines the risk of developing fatty liver disease, but rather an interaction of many genes in your DNA.
Research published in Clinical and Molecular Hepatology describes three genes – PNPLA2, GCKR, and TM6SF2 – that may influence the likelihood of fat accumulation in the liver. Specific variants of each gene are associated with increased risk of conditions associated with fatty liver disease, such as insulin resistance and type 2 diabetes. Of the three genes, PNPLA3 is the most well-studied gene and directly plays a role in liver metabolic processes. Moreover, a certain variant of the PNPLA3 gene is associated with a higher risk of fatty liver disease progression to NASH, fibrosis, and cirrhosis. (1)
Expression of the Fatty Liver Disease Gene Depends on Environment
Your DNA – an abbreviation short for deoxyribonucleic acid – is a code that makes you human and determines your individual traits. Some traits, such as eye color, are influenced by just two genes and based on your inherited genes, will remain set in stone for your lifetime.
Other traits, such as personality, are much more complex and described as polygenic traits since they are influenced by a large number of different genes. An individual’s personality – like introversion or open-mindedness – is highly influenced by both genes and the environment. For example, a naturally introverted child may become more extroverted over time in response to positive experiences with family and peers.
The expression of the genes contributing to fatty liver disease is comparable to more complex traits, like personality. Inheriting certain forms of the gene may predispose you to fatty liver disease under certain environmental conditions.
Influence Your Genes with Diet and Lifestyle
Even if you have a gene that predisposes you to fatty liver disease, you are not destined for liver problems. Diet and lifestyle can influence your genes for better or for worse. If you have the fatty liver disease gene, your diet and lifestyle can prevent the expression of these genes.
Conversely, you don’t have to have the fatty liver disease gene to develop fatty liver disease. If you don’t have the fatty liver gene, certain diet and lifestyle factors cause the development of fatty liver disease. Generally, a sedentary lifestyle and diet high in added sugars and saturated fat can induce epigenetic changes that accompany fatty liver disease.
A study conducted by researchers at the Department of General and Thoracic Surgery at the University Hospital Schleswig-Holstein in Kiel, Germany, assessed the DNA of patients with fatty liver disease before and after bariatric surgical treatment for weight loss. The analysis showed that genetic changes associated with fatty liver disease were reversed post-treatment, revealing the liver’s ability to respond positively to environmental changes. (2)
Managing Fatty Liver Disease
The management of nonalcoholic fatty liver disease depends primarily on making changes to your diet and lifestyle. In some cases, your physician may prescribe medications like metformin and statins to help concurrent metabolic conditions like insulin resistance and high cholesterol.
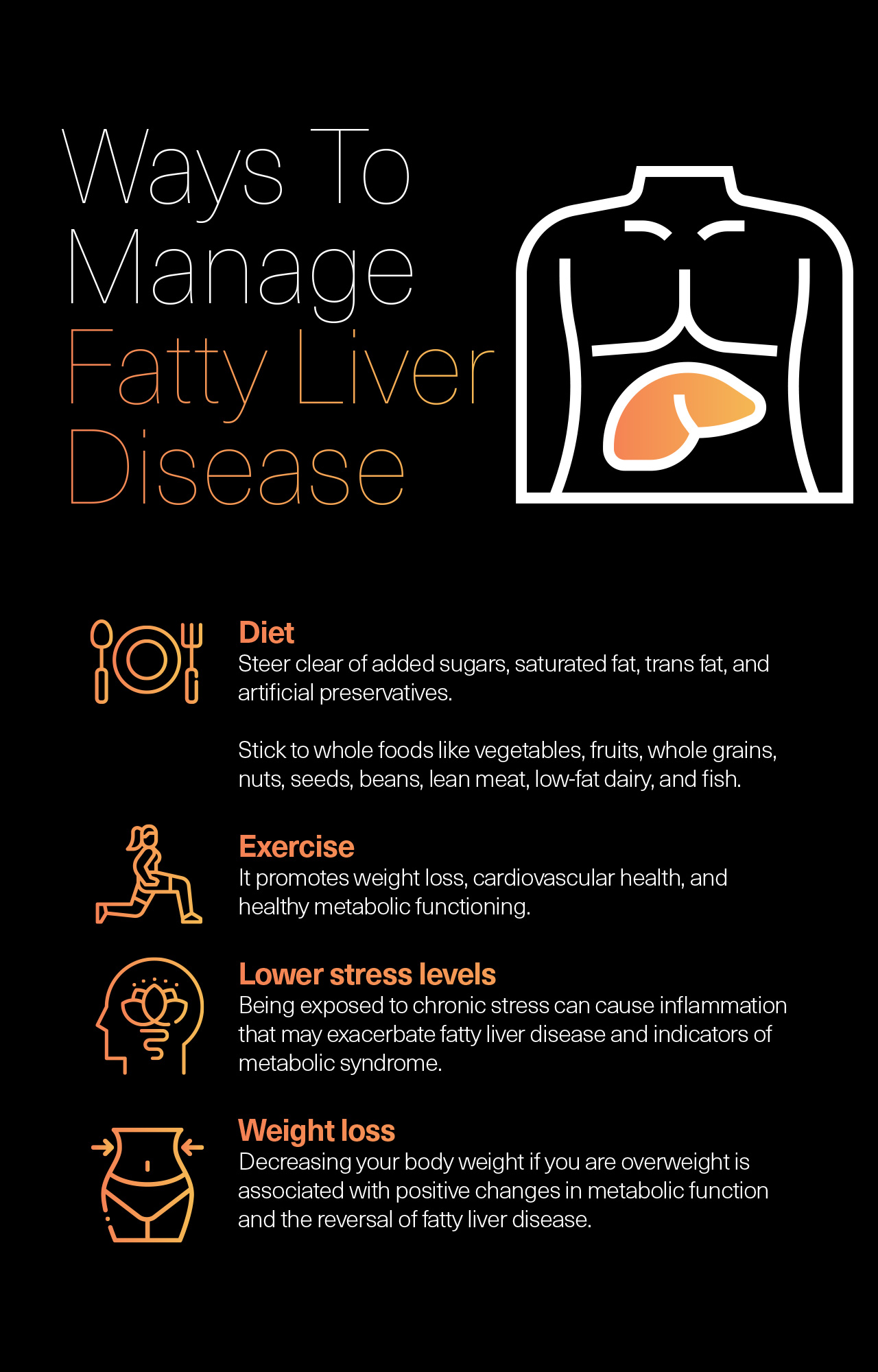
Diet
Food can help you change how your DNA is expressed and following a hepatic steatosis diet can help reverse fat accumulation in your liver. To lower the risk of developing fatty liver disease, it is important to cut out foods that inhibit healthy metabolic function and negatively alter the expression of genes that play a role in metabolic processes.
Steer clear of added sugars, saturated fat, trans fat, and artificial preservatives. Instead, stick to whole foods like vegetables, fruits, whole grains, nuts, seeds, beans, lean meat, low-fat dairy, and fish. Eating these foods will ensure that you get optimal amounts of fiber, complex carbohydrates, and essential amino acids needed to power biological functions. Whole plant foods like leafy greens and fruit afford an abundance of micronutrients- like vitamin E, vitamin C, and polyphenols- that exhibit antioxidant and anti-inflammatory activity. Such micronutrients play a role in reversing fatty liver disease, improving insulin sensitivity, and lowering blood pressure.
It’s important to make sure that when following a diet plan, you make sure it’s tailored to best support the reversal of fatty liver disease. There are many fad diets out there – like the paleo diet, low-fat diet, low-carb diet, vegan diet, and the Mediterranean diet – that may have many positive premises but need adjustments to most effectively address fatty liver disease and metabolic function. Just make sure you are equipped with all the information you need to make healthy food choices that support your liver and metabolic health.
Exercise
Exercise promotes weight loss and cardiovascular health. Aerobic exercise is particularly important for increasing cardiovascular health since it strengthens the heart and blood vessel function. This, in turn, leads to better blood flow and lower blood pressure.
Strength training is equally important. Regular strength training helps build and maintain lean muscle mass. Having lean muscle mass boosts your resting metabolic rate and helps promote healthy metabolic functioning.
Start out slow and gradually increase your exercise levels, allowing your body to adjust to your new lifestyle. It’s helpful to have a workout plan that you enjoy so you can stick to it and see the results you want.
Lowering Stress
Chronic stress has repercussions for health on a physiological level. The stress response increases adrenaline and leads to high levels of serum cortisol and blood sugar. Being exposed to chronic stress can cause inflammation that may exacerbate fatty liver disease and indicators of metabolic syndrome.
Stress is also a major DNA-methylator that can negatively impact many normal biological functions. Strive to incorporate stress management techniques into your daily routine, even if you can only find a few minutes to yourself.
Losing Weight
Decreasing your body weight if you are overweight is associated with positive changes in metabolic function and the reversal of fatty liver disease. As you lose weight, excess fat will disappear from adipose tissue and your liver.
Maintaining a steady calorie deficit is the most effective way to lower your BMI. Individual calorie needs are determined by your individual metabolism, activity level, and any specific needs.
Conclusion
Hepatic steatosis or fatty liver disease is a highly manageable and reversible condition when addressed at early stages. Even if you are genetically predisposed to fatty liver disease, you can make diet and lifestyle changes that positively alter the expression of your DNA and reverse fatty liver. Exercising regularly, cutting out processed foods, and getting a balance of healthy fats, carbs, and essential amino acids are key when it comes to preventing and reversing nonalcoholic hepatic steatosis.
References: