Have you been diagnosed with liver cirrhosis? This is a late-stage liver disease that involves scar tissue replacing healthy liver tissue. It’s critical to know the basics of this serious disease including symptoms, causes, treatments, and prevention. It’s also important to know about possible complications. They include infections, jaundice (yellowish skin/eyes), stomach/leg swelling, and others. These symptoms of complications of cirrhosis can make it tougher to deal with liver disease. So it’s critical to know when you’ve developed symptoms that are among the disease’s complications besides the standard tissue scarring. These toxins can even affect the brain like the condition HE that involves a toxin buildup. This can cause symptoms like confusion.
There are two main types of cirrhosis of the liver. One only involves the disease’s symptoms without any complications. However, there’s also another form of late-stage liver disease that includes various complications. This can make it tougher to treat the health condition based on the particular ones a patient has. Cirrhosis often develops from liver hepatitis, although sometimes it develops directly from fatty liver disease (FLD). It’s late-stage because it involves the liver forming scar tissue to protect itself from damage. The amount of damage is related to the cirrhosis stage the patient is undergoing.
What Is Liver Cirrhosis Really About?
This is a disease that causes scar tissue to replace healthy tissue. This scar tissue prevents blood flow through the vital organ. It also keeps the liver from processing nutrients and hormones, while removing natural/synthetic toxins.
The skin is the body’s largest organ but the liver is the biggest solid organ. The organ has several functions like:
- Breaking down saturated fat
- Making bile for digesting food
- Boosting the immune system
- Making cholesterol
- Storing extra nutrients/returning nutrients to the bloodstream
- Removing alcohol/drugs from the bloodstream
- Helping people store blood sugar
- Producing blood proteins for moving oxygen
The main effect of cirrhosis is the organ is unable to function properly. The most common factors that cause cirrhosis include fatty liver disease (FLD), infections like Hepatitis A/B/C, and heavy alcohol consumption.
There are also various genetic diseases that can cause cirrhosis including:
- Cystic fibrosis
- Heart failure
- Sugar-storage diseases
- Bile duct blockage
- Immune system diseases
- Liver function diseases
There are various other causes of liver cirrhosis. The key is to watch for symptoms, which can be tough. In the early stages there often aren’t any symptoms. So if you experience multiple ones it’s important to get it checked. That’s because there’s a chance you might have later-stage liver disease including cirrhosis.
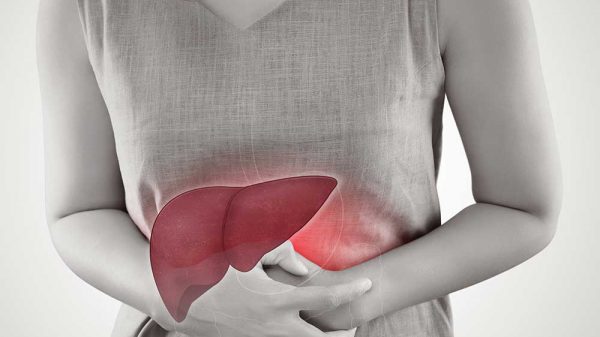
Signs of early-stage cirrhosis include holding onto salt/fluid. This could start as a swollen leg/ankle then move to ascites (fluid buildup in the abdomen). You can treat these symptoms by taking water pills and reducing sodium intake.
In more serious cases, the doctor might have to use a needle to drain some fluid from the stomach. In some cases, the fluid might get infected. This is a symptom that should be dealt with immediately.
When a person has major fluid/water retention they might require a liver transplant. It’s important to talk to your doctor about this procedure.
Top Complications of Cirrhosis
Swelling
This is usually in areas like the abdomen/legs. This results from pressure put on a liver vein. This can result in fluid buildup in the abdomen and legs. Liver disease patients might also have these symptoms when the liver can’t produce enough of some kinds of blood proteins.
Brain Toxins
This condition known as HE results from toxin buildup in the brain when the liver is unable to remove them. The results include a lack of focus and mental confusion. As time passes this can become worse and result in a coma.
Infections
Cirrhosis patients might have problems fighting off infections. Fluid buildup in the stomach can result in a major infection that’s caused by a particular type of bacteria. This can make symptoms worse for cirrhosis patients.
High Blood Pressure
This involves the liver’s veins. When a patient has complications of cirrhosis, it slows down how fast blood flows in the liver. It puts pressure inside the vein that returns blood from the spleen/intestines to the liver.
Malnutrition
Cirrhosis of the liver can make it difficult for the human body to process various nutrients. This can cause weight loss and weakness. That’s because the liver is an important organ in nutrient processing.
Jaundice
This is one of the complications of cirrhosis that happens when a sick liver doesn’t get rid of enough of a waste product in the patient’s blood. It causes yellowish eye/skin.
Bleeding
Hypertension in veins can result in blood being moved to small veins. The small veins could break, which can cause major bleeding. This “portal” high blood pressure can cause big veins in the stomach/throat. If the liver is unable to produce enough clotting this can result in continuous bleeding.
Enlarged Spleen
High blood pressure rein the liver veins can also cause spleen swelling. This results in white blood cells getting trapped. When fewer are in the bloodstream this could be one of the first cirrhosis symptoms.
Top Treatments for Liver Cirrhosis
1. Control pressure on the liver vein
This is known as the “portal” vein. High blood pressure can result from a backup. The vein is critical for supplying blood to the liver. This usually involves prescription drugs to reduce high blood pressure in various blood vessels. The goal is to avoid major bleeding.
2. Liver cancer screening
Patients who have liver cirrhosis have a higher chance of getting liver cancer. Your doctor might order imaging scans and blood tests to check if you have this serious condition.
3. Prescription medications
There are various medications that can help to treat infections like Hepatitis. This can be effective for controlling damage to liver cells. This is critical because Hepatitis can cause liver cirrhosis to progress to more serious stages. This is certainly a situation you’ll want to avoid.
4. Banding
This involves placing a small band around the base of swollen veins in order to reduce bleeding. This can be an effective method for dealing with the problem. Make sure to talk to your doctor if this is a good option for you.
5. Antibiotics
These are prescribed to deal with various infections that take place. Your doctor can inform you about your options and whether there are any side-effects.
6. Stop drinking alcohol
This is critical for alcohol-related cirrhosis. In this case, it’s the alcohol that’s causing your disease. So it’s especially important to ditch or limit alcohol. Since cirrhosis is a late-stage liver disease it’s better to stop drinking completely. This can help to deal with the disease’s various symptoms.
In earlier stages like fatty liver disease (FLD) it’s very practical to limit alcohol. However, if the disease has progressed to liver hepatitis or cirrhosis then you should certainly consider quitting cold turkey or drinking once in a blue moon. This can help to reduce your risk of more liver damage and complications of cirrhosis.