Are you following cirrhosis guidelines? After being diagnosed with late-stage liver disease it’s important to follow them for management/treatment. As much as 10% of the world could have late-stage liver disease. Like the stages of liver disease itself, liver cirrhosis has multiple stages. So it’s important to manage the disease effectively. That, in turn, will help to treat the condition effectively. It’s important to prevent the disease from developing to later stages including liver failure. Taking certain steps can help to prevent the need for a liver transplant, which can cost over $500,000. Besides that, other issues can make the process difficult including finding a donated organ match.
Managing cirrhosis involves slowing down how fast scar tissue forms on the liver. This process is known as “fibrosis” and has become severe by cirrhosis. So it’s important to take steps to prevent the disease from developing to later stages. Stopping alcohol drinking, losing weight, and treating cirrhosis complications are some of the best ways to treat the disease effectively. If you have alcoholic liver disease (ALD) then it’s especially important to ditch alcohol. Maintaining a healthy diet and a healthy lifestyle are some other general ways to prevent liver scarring.
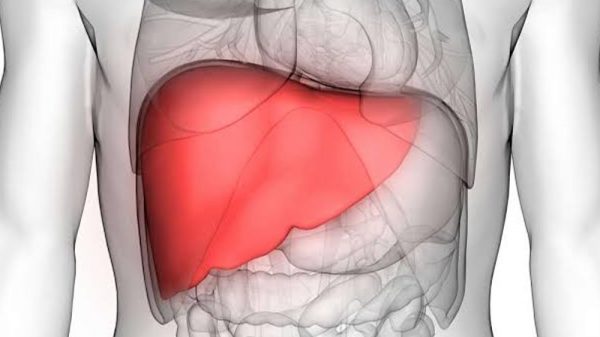
What Exactly Is Liver Disease?
This is the main question to take up before talking about treatment/management. It’s late-stage liver disease, which includes the following stages:
- Stage 1: Inflammation
- Stage 2: Fibrosis (scarring)
- Stage 3: Cirrhosis
- Stage 4: Liver Failure
Before developing liver disease a patient first has a condition known as “fatty liver.” This involves a fat buildup in the vital organ. Over time this can develop into fatty liver disease (FLD). This often develops into scarring of the liver known as “fibrosis.”
If the amount of liver scarring continues it can progress it can lead to cirrhosis. This starts to affect the liver’s functions. In the first stage of cirrhosis, there aren’t any complications. However, that changes as scarring gets worse. This can lead to various related issues including:
- Bacterial issues
- Liver cancer
- Abdominal swelling (ascites)
- Spider web-like blood vessels
- Enlarged spleen
- Swelling of leg/ankle/foot
- Confusion and mood swings (HE)
These conditions can make it tougher to deal with cirrhosis. So it’s important to know the signs/symptoms of complications. This can make it easier to deal with them through management/treatment.
The life expectancy for late-stage liver cirrhosis is up to 2 hours. However, there are various factors including any cirrhosis complications and the availability of a liver transplant.
However, a transplant can cause new issues including maximum costs of over half a million US dollars. There are also more liver transplant candidates than donors.
Your “MELD” score affects your position on the waiting list. In some cases, a liver disease patient’s organ isn’t scarred enough to qualify them for an organ transplant.
There’s no “cure” for liver cirrhosis except for a transplant. However, it’s still possible to take steps to slow down the process of healthy tissue turning into scar tissue. It’s also important to deal with any complications as effectively as possible since they can make management/treatment even tougher.
Cirrhosis Guidelines: Management
1. Lose weight
If you have cirrhosis due to non-alcoholic fatty liver disease (NAFLD) then weight loss might be helpful. There are various reasons with the main one being overall fat loss can also reduce liver fat. Fun Fact: 1 pound of body fat is equal to 3,500 calories. Weight loss not only can improve liver function but also boost overall health.
2. Blood test
These are important for various purposes. For example, it’s important for monitoring other conditions like liver cancer. This is another serious liver disease so it’s critical to get blood work done to check if there are any signs of liver cancer.
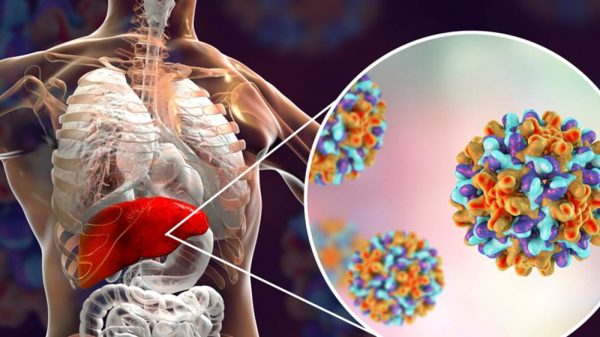
The blood tests can also help to check for various related infections like Hepatitis B/C. When the body is less effective at getting rid of toxins this increases the risk of infections like Hepatitis B/C. It’s important to get blood tests to find out if you’ve been infected. You should also take steps like avoiding risky behavior, to help reduce your chance of getting hepatitis.
3. Follow the low-sodium diet
This is something you should consider anyway. The American Heart Association (AHA) recommends adults consume less than 1500mg of sodium per day. Sodium can add up quickly during the day. One tablespoon of soy sauce can have up to 1000mg.
If you have abdominal fluid buildup (ascites) then it’s especially important to limit salt intake. A high-sodium diet can cause fluid buildup, which can trigger ascites symptoms.
4. Limit/Quit alcohol
If you have alcoholic liver disease (ALD) then it’s critical to quit alcohol cold turkey. Even a moderate amount of alcohol could cause more damage to your vital organ. Various non-alcoholic drinks can produce similar effects without actually consuming beer, wine, or spirits. Some recent studies show that drinking alcohol daily seems to be a myth.
Cirrhosis Guidelines: Treatment
1. Immune System Problems
Sometimes some complications cause your immune system to attack healthy cells. This can cause various complications that require treatments. For example, this can involve the blockage of the bile duct. Another related issue is when hepatitis affects the immune system. In both situations, it’s important to deal with the immune system conditions.
2. High Blood Pressure
One complication that can result from cirrhosis is high blood pressure in the liver’s veins. This is a condition that should be treated like others to make the liver disease more manageable. It’s important to get checked out for this condition so it can be treated if necessary.
3. Spider web-like blood vessels
This happens when the blood vessels expand too much then start to bleed. This condition should be treated with a rubber band or a surgical procedure known as TIPS.
4. Hepatitis Treatment
Hepatitis B/C can trigger liver damage and lead to cirrhosis within time. There are various treatments you can receive like anti-viral medicines. In many cases, these medications can cure the infection. If you have Hep A/B/C it’s important to talk to your doctor about prescription meds you can take.
5. Hepatic Encephalopathy (HE)
This mental condition results from toxin buildup in the blood due to health conditions like late-stage cirrhosis. This can cause various results like lack of focus, memory loss, and mental confusion. This condition can be prevented/treated by taking medicines to reduce blood toxins.
6. Alcohol Addiction Treatment
If you have a problem with heavy drinking it’s important to quit ASAP. There are various resources available. They include programs like Alcoholics Anonymous (AA), therapist counseling, support groups, and rehab programs.
It’s important to view alcoholism as a disease that requires treatment. In the case of liver disease, it’s especially important to ditch alcohol since it’s caused tissue scarring on the liver and part of cirrhosis guidelines.