Medically ascites is defined as fluid accumulation in the peritoneal cavity. Several conditions and diseases can lead to ascites, for example, abdominal cancer, liver cirrhosis, tuberculosis, and congestive heart failure. Ascites physical exam involves checking the patient for physical symptoms of fluid accumulation. Symptoms and signs of ascites include bloating, liver failure, bloating, and short breath. Ascites treatment involves managing or curing the underlying health condition which may include avoiding alcohol, limiting fluid intake, limiting salt intake, and some other changes to your lifestyle. Some complications may result from ascites such as lower intestine bleeding, kidney failure, and liver cirrhosis complications.
Ascites are traditionally divided into two types; exudative or transudative. The basis for this classification is the protein amount contained in the accumulated fluid. A useful system known as serum ascites albumin gradient was developed from the ascitic fluid albumin amount compared to albumin in serum. Ascites that are related to the high pressure of the portal venous system is typically more than 1.1 while ascites developed by different reasons like pancreatitis, malignant is less than 1.1.
Ascites Physical Exam
Ascites diagnosis relies on conducting a physical exam in relation with the medical history of the patient in order to determine the underlying possible health issues since ascites is usually considered to be an indirect symptom of other health conditions. Ascites fluids that measure more than 500ml can be seen on physical exams by fluid waves and bulging flanks performed during the abdomen examination.
Ultrasound may detect smaller fluid amounts. A regular CT scan or an ultrasound can find ascites accidentally. It is very important to get the correct diagnosis of underlying health issues that caused ascites as this will help in understanding why the person developed ascites. Reviewing the patient’s medical history may supply clues to get the underlying health issues.
The doctor will ask questions concerning previous liver disease diagnosis, viral hepatitis, alcohol abuse, heart failure, medication history, and cancer history.
Blood tests may play important roles in ascites cause evaluation. A completed detailed metabolic panel is able to detect liver injury patterns electrolyte levels, kidney, and liver functional status. CBC is also beneficial in determining underlying conditions. Coagulation panel abnormalities may exist due to inadequate protein clotting production.
Sometimes the underlying ascites causes may not be gotten by physical exam, history taking, or reviewing imaging studies and laboratory data. The fluid analysis may also be needed so as to gain more diagnostic data. This is a procedure known as paracentesis which is carried out by skilled trained physicians.
Paracentesis involves sterilizing a particular abdominal area and using ultrasound guidance to insert a needle in the cavity of the abdomen and withdraw fluid for more analysis.
Ascites Symptoms
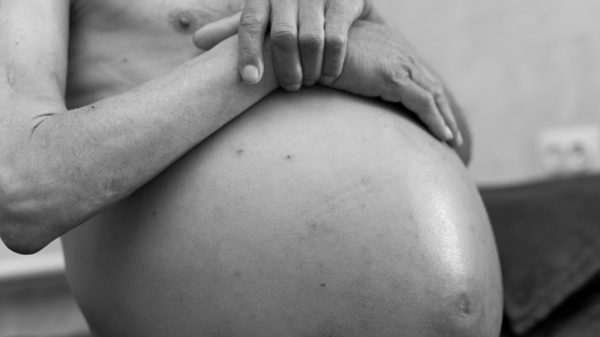
No symptoms are associated with ascites particularly when the ascites are mild, which is less than 100-400 for adults. With the accumulation of more fluid, there will be a corresponding increase in abdominal girth and size.
Bloating, discomfort and abdominal pain are the common ascites symptoms experienced as the ascites grow bigger. Breath shortness may also occur with big ascites as a result of increasing pressures on the body’s diaphragm and fluid migration across this diaphragm leading to pleural effusions that are fluids around or in the lungs. Most patients are concerned about the cosmetically disfigured state of their large belly.
Ascites Treatment
The underlying health condition will determine the course of ascites treatment. For example, malignant ascites or peritoneal carcinomatosis can be treated surgically by resecting cancer and also chemotherapy while ascites management linked with failure of the heart is focused on treating the heart condition with dietary restrictions and medical management.
Ascites patients have special diets .they are to restrict their sodium(salt) intake and taking diuretics. The practical way of reducing dietary salt intake is to lower than two grams daily. However, in most cases, the use of diuretics and restricted sodium intake may not be effective in treating ascites.
Medications
A diuretic increases salt and water excretion via the kidneys. Aldactone (spironolactone) and Lasix (furosemide) are two recommended diuretics. 40 mg of furosemide and 100 mg of spironolactone are the ideal first dosage. It can be increased gradually in order to get the correct response to 160 mg for furosemide and 400mg which is the highest dosage for spironolactone.
These doses will only be given if the patient is able to tolerate the increased dose without exhibiting side effects. It is usually better to take the medication at the start of your day to avoid urinating frequenting at night.
Ascites Complications
Some ascites complications may be associated with its amount. The fluid accumulation may lead to difficulty in breathing due to pleural effusion formation or diaphragm compression.
Another severe ascites complication is infections. In patients with portal hypertension ascites, gut bacteria may invade ascites fluid spontaneously causing an infection. A condition is known as SBP or spontaneous bacterial peritonitis. Ascites rarely contain antibodies and thus its fluid is with limited immune response.
SBP is diagnosed by paracentesis and fluid analysis for the amount of WBCs or bacterial growth evidence.
A potentially deadly condition is the hepatorenal syndrome which can be an ascites complication and is related to liver cirrhosis causing the progressive failure of the kidney. Scientists are yet to discover this syndrome exact mechanism but it is suspected that it is caused by fluids shift, a diuretic overuse, administering IV contrast, and impaired kidney blood flow.
Summary
Ascites in itself are not life-threatening but its cause might be hence it should be treated as a serious health condition.
After conducting an ascites physical exam, the doctor should verify the diagnosis and place the patient on the available and effective treatment option addressing the health issue. if you have a family history of liver damage and are worried about the chances of getting sick, you can go for a check-up. If your liver is healthy still maintain a clean and healthy lifestyle for the sake of maintaining your liver health.